Yellow jaundice in newborns is one of the most common conditions after birth, as yellowing of the skin and yellowing of the whites of the eyes of the newborn is observed as a result of the accumulation of bilirubin in the blood.
Sometimes the yolk is normal and temporary, but sometimes it may indicate a problem that requires urgent medical intervention.
Through this article, Almoosa Hospitals provides a detailed explanation to understand the causes of jaundice, its types, and safe methods of prevention and treatment.
What is the definition of yolk in newborns?
Jaundice (jaundice) in newborns is common in the first days after birth;
After birth, the infant's liver gradually begins to process this substance;
Types of yolk in newborns
Neonatal jaundice is divided into several types according to the cause and nature:
- Physiological yolk:
It is the most common and usually appears between the second and fourth days after birth, and results from the immaturity of the infant’s liver.
- Pathological yolk:
It appears in the first 24 hours after birth or is very severe, such as yellowing of the palms of the hands and soles of the feet.
- Early breastfeeding yolk:
It occurs when the newborn receives a small amount of breast milk in the first days, which reduces the excretion of bilirubin with feces and urine.
- Breast milk yolk:
It sometimes appears after the first week of birth, as a result of natural substances in breast milk that increase the absorption of bilirubin.
- Direct bilirubin and indirect bilirubin:
Yolk Unconjugated (Indirect) is the most common and includes the previous types. conjugate (direct) It indicates a problem with the liver or bile ducts and requires in-depth medical evaluation.
- Other rare species:
Such as jaundice resulting from congenital problems in the liver or bile ducts, or jaundice associated with neonatal infections.
Most cases of neonatal jaundice are physiological and resolve without intervention within a few weeks, while severe or early jaundice requires urgent medical attention to ensure the safety of the infant.
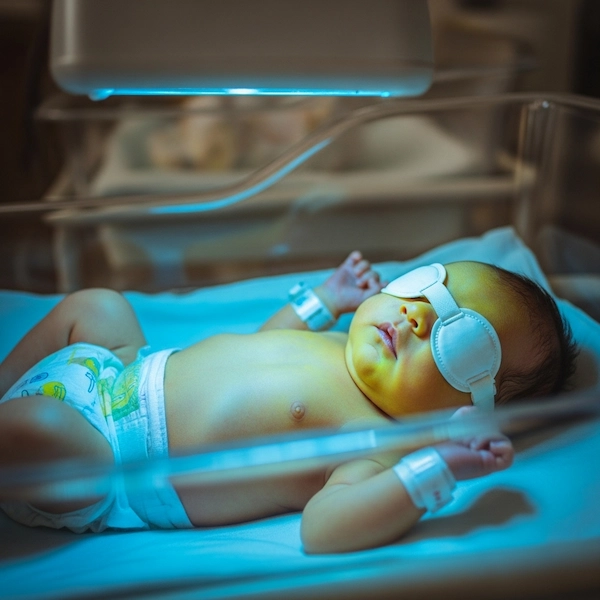
Causes and factors contributing to the occurrence of jaundice in newborns
There are several factors that increase the risk of jaundice in newborns. Among them:
- Liver immaturity:
As the newborn's liver has not yet fully developed;
- Increased hemolysis:
In cases of birth bruises or subcutaneous bleeding, the breakdown of red blood cells increases, which raises the level of bilirubin in the baby's blood.
- Blood incompatibility of mother and child:
If the mother's blood types are different (such as a different RH factor or A/B blood groups), the mother's system may attack the infant's blood cells in the womb or after birth, causing a rapid rise in bilirubin.
- Premature birth:
Babies born before 37 weeks of pregnancy are more susceptible to jaundice, because their liver is still weak at processing bilirubin.
- Inadequate nutrition:
If the infant does not get enough milk (especially in the first days), the excretion of bilirubin in the stool and urine decreases.
- Deficiency of certain enzymes or genetic conditions:
Such as G6PD enzyme deficiency or other metabolic disorders, which may lead to high bilirubin and the appearance of jaundice.
- Infections and diseases:
Some bacterial or viral infections in newborns (such as a urinary tract infection or hepatitis) can cause high bilirubin.
- Bile pathway problems:
Biliary obstruction or congenital liver disease may cause bile to accumulate within the liver, causing conjugated jaundice.
Learn about: Vaccination program at Almoosa Health Hospitals
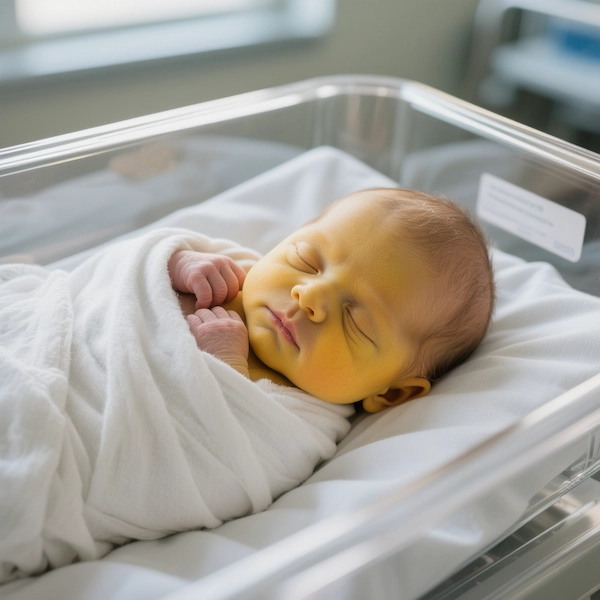
Yolk signs in newborns
The most important sign of yolk is yellowing of the newborn's skin and the whites of his eyes. Symptoms associated with yolk include:
- Yellowing of the face and eyes:
It appears on the cheeks, forehead, and whites of the eyes, then extends to the chest and limbs.
- Change in color of urine and stool:
In severe jaundice, the color of the child's stool may become pale or gray, and parents may notice an increase in the color of the urine.
- General symptoms:
Severe yolk may be accompanied by poor appetite, difficulty feeding, and excessive sleepiness..
When is yolk dangerous for the infant?
There are signs that the yolk may be dangerous and requires immediate medical attention, Among them:
- Early appearance of yolk:
If yolk appears within the first 24 hours after birth, this usually indicates a serious medical condition that requires immediate examination.
- Severe or prolonged yellowing:
If parents notice dark yellowness extending to the palms of the hands and the soles of the feet, this indicates a significant increase in the level of bilirubin.
- The yolk persists for a long time:
Skin yellowing that persists for more than two weeks (or more than three weeks in premature infants) warrants medical evaluation.
- Poor lactation and hydration:
If the baby is very lethargic or is urinating and defecating less than normal (less than 4 wet diapers a day), this could mean dangerously high yolk.
- Behavioral or neurological changes:
Excessive sleepiness, difficulty waking up, high-pitched crying, or the appearance of stiffness in the body's muscles may indicate the effect of the yolk on the nervous system, and you should consult a doctor immediately.
- Other worrying symptoms:
Such as a child’s high temperature or the appearance of a skin rash accompanied by jaundice that requires urgent review.
Methods of diagnosing jaundice in newborns
Diagnosis of jaundice in newborns includes a clinical examination and simple blood tests:
- Physical examination:
The doctor checks the nature of the color of the child's skin and the whites of his eyes to estimate the presence and degree of yolk.
- Measuring bilirubin levels:
A device can be used to measure bile levels non-invasively, or a simple blood sample can be drawn to measure total and direct bilirubin in the laboratory.
- Additional tests:
If the jaundice is severe or early, the doctor may order additional tests to determine the cause, such as blood type testing, Coomb’s test for blood compatibility, or tests to detect hereditary conditions or thyroid problems.
How do I treat jaundice in newborns?
How to treat jaundice depends on its severity and cause. It may include:
- Phototherapy:
It is the main treatment for most cases of jaundice.
- Blood transfusion:
In severe cases that do not respond to phototherapy alone, the doctor may perform a blood exchange.
- Addressing the cause:
If the jaundice is caused by immune hemolysis (blood type difference), your doctor may prescribe immunoglobulin injections (IVIG) to reduce the breakdown of blood cells.
- Nutrition and hydration support:
The doctor recommends that the child breastfeed frequently (8-12 times a day) to ensure that he receives sufficient amounts of milk.
Almoosa Hospitals offers modern phototherapy units in its neonatal departments to ensure that phototherapy is administered effectively and comfortably within a safe medical environment.
How do I treat jaundice in newborns at home after a medical examination and treatment?
After undergoing a medical examination or receiving treatment, Parents can follow some guidelines at home to help the baby recover and monitor the yolk:
- Increase lactation and hydration:
Focus on breastfeeding the child frequently and ensuring that he receives a sufficient amount of milk and only permitted fluids.
- General condition monitoring:
Monitor the child's weight regularly to ensure that he is gaining the required weight, and note the number of wet diapers and the number of times he defecates.
- Check skin color daily:
It is preferable to examine the child's skin in natural daylight.
- Rest and avoid stress:
The child should be kept comfortable in a moderate temperature environment, avoiding excessive heating or cooling.

Note!!
Mild physiological jaundice does not cause any serious complications if appropriate treatment is followed.
Complications include impaired hearing or vision, delayed mental or motor development (such as cerebral palsy), and sometimes tooth discolouration. Liver functions And its general growth.
Fortunately, with early testing, most children recover without any side effects.
Table of jaundice levels in newborns
| The child's age in days | Normal rate (mg/dL) | Condition and medical evaluation | General recommendation |
| During the first 24 hours | Less than 5 mg/dL | A height higher than this is considered abnormal and often indicates pathological jaundice | It needs immediate examination by a doctor |
| Day 2-3 | From 5 to 12 mg/dL | Yolk is considered normal physiological function in most healthy newborns | Just follow up and increase breastfeeding |
| Day 4-5 | Up to 15 mg/dL | Acceptable in full-term newborns, but caution should be exercised in premature infants | Continuous monitoring, and phototherapy if increased |
| After day 7 | Less than 10 mg/dL | The continued increase in the percentage after the first week requires evaluation | Additional examination To find out why |
| After the second week | Any rate above 5 mg/dL | If the yolk persists for this period of time is considered abnormal | See a doctor to examine the liver and blood |
FAQs
When does the yolk disappear in newborns?
Physiological yolk usually disappears within one to two weeks after birth.
Does jaundice cause death in newborns?
In very rare cases, jaundice may cause death in newborns, and this often occurs due to neglecting to measure the high percentage of yolk, despite the appearance of symptoms on the child and a change in the color of the face and skin..
Why does yolk persist in infants for more than two months?
The continuation of yolk for more than two months requires urgent medical advice, as it may indicate disorders in the liver, bile ducts, or thyroid gland.
Conclusion
Jaundice in newborns is a common condition that is easily treatable when detected early. Almoosa HospitalsYou can be assured of your children's health through the latest methods of diagnosis, treatment, and specialized care for newborns.
Do not hesitate to book an appointment or visit the nearest branch of our hospitals to check on the health of your liver and receive accurate medical instructions to protect it from any future complications.
Read also: Al-Moussa programs for the rehabilitation of speech, speech and communication disorders
