Testicular cancer represents only about 1% of all types of cancer that affect men, but it is the most common among males between the ages of 15 and 35 years. However, the cure rate for seminoma tumors may reach 99%, and through Al Mousa Specialist Hospital we offer you this comprehensive medical guide;
What is testicular cancer?
Testicular cancer is one of the types of cancer that originates in the cells of the testicles, which are the two organs responsible for producing sperm and male hormones. Testicular cancer usually affects young and middle-aged men, and is often treatable if detected early.
The most common types of testicular cancer
The most common types of testicular cancer are divided into two main types, both of which arise from germ cells. They are the most common in testicular cancer, and they are as follows.
1. Seminomas
- They grow relatively slowly.
- It usually affects men between the ages of 30 and 50.
- More responsive to radiotherapy and chemotherapy.
- It is often detected in the early stages.
2. Non-seminomas
- It includes multiple types such as embryonal carcinoma, yolk sac tumor, choriocarcinoma, and teratoma.
- It tends to grow and spread quickly.
- It usually affects younger men between 20 and 35 years of age.
- Less responsive to radiotherapy but chemotherapy is effective.
What are the causes of testicular cancer?
The causes of small testicular cancer are still not definitively known, but medical studies have identified a number of factors that may contribute to increasing the probability of developing this type of cancer, the most prominent of which are:
- Cryptorchidism: It is a condition in which one or both testicles do not descend into the scrotum at birth, and this condition is considered one of the strongest risk factors, even if it is corrected surgically at a later time.
- Family history: The presence of previous cases in the family, such as a father or brother, which increases the risk of infection in other family members.
- Race: White men are more likely to develop testicular cancer than men of African or Asian descent.
- the age: Testicular cancer is most common in males between the ages of 15 and 35, but it may occur at any age.
- Previous injury: If a person has previously had cancer in one testicle, this increases the risk of developing it in the other testicle.
- Infertility and poor fertility: Some studies indicate a link between fertility problems and an increased risk of testicular cancer, but this is not entirely certain.
- Some genetic syndromes: Like Klinefelter Syndrome, it may be a factor associated with an increased risk of infection, although it is rare.
Risk factors that increase the likelihood of infection
As we mentioned, there is no specific direct cause for testicular cancer, but there are several factors associated with increasing the probability of infection, including:
- Undescended testicle is the failure of one or both testicles to descend into the scrotum.
- Family history and the presence of previous cases of cancer in the family.
- Previous history of testicular cancer increases the risk of infection in the other testicle.
- Age: It most often affects men between 15 and 35 years old.
- Some genetic syndromes such as Klinefelter syndrome.
- Repeated injuries or infections may play a role in increasing the risk.
- Environmental factors such as exposure to chemicals or industrial hormones.
Learn about: Causes of varicocele Causes and how to diagnose
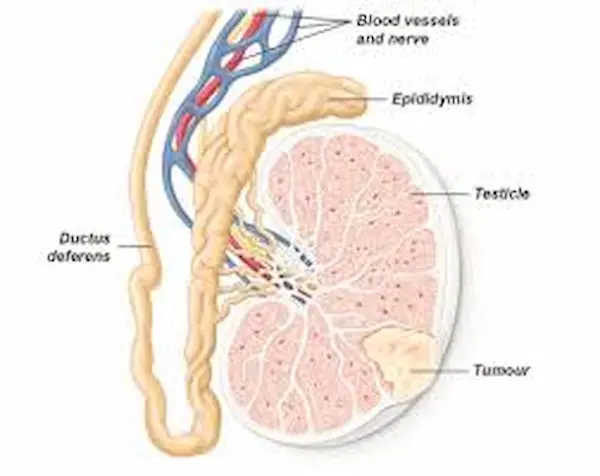
Common symptoms to watch out for
Early detection of testicular cancer is crucial to increasing the chances of recovery, so it is necessary to know the symptoms that may indicate the presence of a problem. The following are the most common symptoms that require attention:
- The presence of a mass or swelling in the testicle is one of the most obvious and common symptoms. The mass is often painless but can be felt when touched.
- A feeling of heaviness in the scrotum, where the patient may feel that the testicle is heavier than usual, for no apparent reason.
- In some cases, the tumor is accompanied by mild pain or discomfort in the lower abdomen or in the scrotum.
- A change in the size or shape of one of the testicles, such as sudden enlargement or gradual atrophy.
- Sudden accumulation of fluid in the scrotum, which shows an unusual increase in the size of the sac.
- Pain in the back or in the area between the abdomen and thigh. This symptom may indicate the spread of the disease to the lymph nodes in the back of the abdomen.
- Breast enlargement or pain, but this is rare, as in certain cases some tumors can cause hormonal changes that lead to breast tissue enlargement.
The appearance of any of these symptoms does not necessarily mean the presence of cancer, but they are warning signs that require consultation with a specialist doctor to conduct the necessary tests. Through the Oncology Center at Al Mousa Specialist Hospital, we help you with a thorough examination, using the latest devices to diagnose the condition, and then develop the appropriate treatment plan.
Stages of testicular cancer development
The classification of the stages of testicular cancer depends on the extent of the disease’s spread in the body, which is used to determine the appropriate treatment plan. The stages are divided into three main stages according to the TNM system, which includes the size of the tumor and the extent of its spread to the lymph nodes or other organs.
Stage I
- The cancer is confined to the testicle only, and has not spread to the lymph nodes or the rest of the body.
- This stage is the simplest and most treatable.
Stage II
- The cancer spreads from the testicle to the lymph nodes, in the back of the abdomen and the lumbar region.
- This stage, in turn, is divided into subgrades, depending on the number and size of affected nodes.
Stage III
- The cancer may have spread to other distant organs, such as the lungs, liver, and rarely the brain.
- This stage is more complex and requires more comprehensive treatment.
Book your consultation now at Oncology center At Al Mousa Specialist Hospital.
Treatment methods available for testicular cancer
Testicular cancer treatment depends primarily on the type of tumor, its stage, and the extent of its spread, and aims to completely eliminate the cancer cells while preserving as much as possible fertility and quality of life. The main treatment options include the following.
1. Surgery (surgical resection)
- It is the initial and basic treatment in most cases of testicular cancer.
- The entire affected testicle is removed in a procedure known as radical inguinal orchiectomy.
- In some advanced cases, the lymph nodes in the abdomen may also be removed, especially in non-seminomas.
- An artificial testicle can be implanted for cosmetic purposes if the patient desires.
2. Chemotherapy
- It is used to destroy cancer cells that have spread outside the testicle or to prevent the disease from returning after surgery.
- Most effective in cases of non-seminomas that spread rapidly.
- It is given to the patient in intravenous courses.
- It usually involves a combination of medications such as cisplatin, etoposide, and bleomycin.
- Its temporary side effects include hair loss, nausea, and fatigue.
3. Radiation therapy
- It is particularly used to treat seminomas that are more responsive to radiation.
- It aims to destroy cancer cells remaining in the lymph nodes after surgery.
- Radiation is applied to specific areas in the abdomen or pelvis.
- It is not usually used in nonseminomas because they are resistant to radiation.
We also note that a combination of these treatments may be used depending on each case. Fertility may also be affected by treatment.
Tips for prevention and early detection
Although there is no guaranteed way to prevent testicular cancer, early detection contributes greatly to raising cure rates and reducing the progression of the disease, as testicular cancer is one of the most responsive types of cancer to treatment, especially if it is discovered early. Here are several tips for prevention and early detection:
- Regular self-examination of the testicles is recommended to be performed once a month, especially after a warm shower when the testicles are in a relaxed state. Each testicle is gently examined using the fingers to look for any mass, or abnormal change in size or shape.
- Pay attention to any unusual symptoms, such as the appearance of a painless mass, heaviness in the scrotum, or pain in the lower abdomen. If you notice any of these symptoms, you should see a doctor immediately.
- Ensure medical follow-up if there are risk factors such as the presence of a previously undescended testicle or a family history of infection. It is also recommended to conduct periodic examinations at Al Mousa Specialist Hospital even if no symptoms appear.
- Maintaining a healthy lifestyle. Although there is no confirmed direct relationship between lifestyle and testicular cancer;
Frequently asked questions about testicular cancer
Does testicular cancer affect fertility?
Yes, it may affect fertility, especially if the treatment includes surgery to remove the testicles or the use of chemotherapy or radiation, but many patients are able to conceive after treatment, and it is recommended to preserve sperm in advance when needed.
What is the difference between benign and malignant swelling in the testicle?
Benign swelling does not spread to other parts of the body and usually does not pose a significant risk, while malignant, cancerous swelling can grow quickly and spread to the lymph nodes or other organs if not treated early.
How do I know that I am free from testicular cancer?
It is possible to ensure through regular self-examination that there are no abnormal lumps or swellings, in addition to performing medical examinations such as x-rays and blood tests when in doubt, and it is necessary to consult a specialist doctor to accurately evaluate the condition.
Does testicular cancer cause death?
Yes, testicular cancer can cause death if it is not detected and treated in its early stages, but it is also one of the most curable types of cancer, and the cure rate exceeds 95% when detected early.
How often does a testicular mass become cancerous?
About 4 out of every 10 masses discovered in the testicle are non-cancerous, but it is always recommended that any mass be considered malignant until proven otherwise by testing.
in conclusion;
المصادر:
Testicular cancer – clevelandclinic
What Is Testicular Cancer? – verywellhealth
Testicular Cancer Statistics – hopkinsmedicine
