Nervous eczema is one of the annoying skin conditions that greatly affects the daily life of the individual who suffers from it. It is linked to the psychological state and constant tension, and its symptoms are chronic and severe itching and thus excessive scratching, which leads to inflammation and changes in the skin such as redness and thickening of the skin. It appears in specific areas such as the neck or extremities, and it is linked to various psychological factors such as anxiety and nervous pressures, which makes its treatment require a balance between skin care, psychological support, and control of stress and emotions, as follows with Al Mousa Specialist Hospital.
What is neurogenic eczema?
قبل أن نلقي الضوء على تفاصيل الإكزيما العصبية من الأسباب والاعراض وطرق العلاج، دعونا نتعرف على ماهية هذا المرض، فإن الإكزيما العصبية هي حالة جلدية مزمنة غير معدية معروفة طبيًا بإسم التهاب الجلد العصبي، وفيها تظهر بقع محددة من الجلد الجاف السميك المصحوب بحكة شديدة بسبب الحك أو الفرك المتكرر، وهي حالة عصبية تنتج عن عوامل نفسية مختلفة مثل التوتر والقلق والضغوط العصبية، وهي تبدأ بحكة خفيفة وتتطور مع مرور الوقت إلى التهاب شديد بسبب الاستجابة العصبية الزائدة، كما تظهر
Who are the people most vulnerable to it?
Of course, you ask yourself: Am I one of those people who are susceptible to infection? Whether you are worried about your infection or the infection of someone close to you, do not worry. There is a list that includes people who are most at risk of developing neurogenic eczema, which is as follows:
- Those who suffer from chronic anxiety or stress, as psychological stress is one of the most prominent triggers for the condition to begin or worsen.
- For those with a prior history of anxiety disorders or depression, psychological factors play a large role in the development and persistence of neurogenic eczema.
- Those suffering from other skin conditions such as atopic eczema or psoriasis, where their skin is more sensitive and responsive to irritation.
- Those who live in an environment full of psychological pressure or stressful work conditions, such as those working in high-pressure jobs or in a psychologically unstable environment.
- Individuals who have frequent habits of scratching or rubbing the skin when stressed, as this behavior turns into a habit that leads to skin damage and worsens the condition.
- Women are slightly more susceptible than men, due to hormonal changes that may affect psychological state and skin response.
Symptoms of neurogenic eczema
Symptoms of neurological eczema include a group of skin and psychological signs that appear locally and chronically. The symptoms may worsen with psychological stress, anxiety, or lack of sleep, and continue for long periods unless appropriate treatment is intervened. The most prominent of these symptoms are as follows:
- Severe and continuous itching, which is the main symptom and increases during periods of stress or before sleep.
- Thick, dry patches of skin resulting from repeated scratching. This condition is known as lichenification.
- Redness and irritation in the affected area, which may sometimes be accompanied by peeling or cracking of the skin.
- Change in skin color, where it becomes darker or lighter than the normal skin color in the affected areas.
- Repeatedly scratching involuntarily turns into a nervous habit that is difficult to stop, which increases skin irritation.
- The appearance of spots of a specific shape and size, usually on the neck, wrists, ankles, behind the knees, or scalp.
- Temporary relief after scratching is followed by an increase in the intensity of itching later, which leads to worsening of the condition.
Read also: تشخيص أمراض الجلد وأبرز أسباب الإصابة
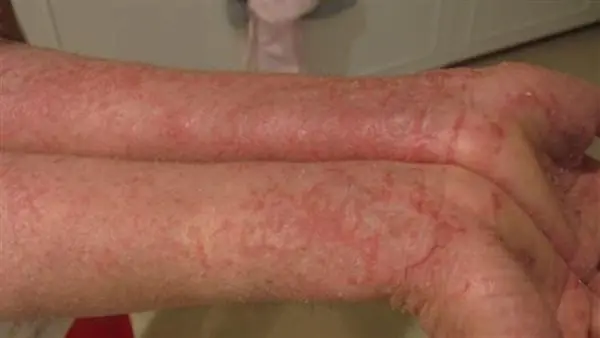
Locations of neurogenic eczema
Nervous eczema appears in specific areas of the body that are more susceptible to frequent scratching, and these places are often easy to reach with the hand. The most prominent locations of its appearance are:
- The back of the neck is one of the most common places, especially with tension or sweating.
- Wrists and backs of hands due to excessive friction and daily movement.
- Ankles and feet, especially when wearing uncomfortable shoes or with excessive sweating.
- The arms and legs are on the outer sides, where the hand can easily reach them for scratching.
- The scalp causes chronic itching, and it is difficult to distinguish neurogenic eczema from normal dandruff.
- The upper chest or back in conditions related to stress or excessive sweating.
- The genital area or inner thighs are more embarrassing for the patient and may have a significant psychological impact.
Factors that increase the probability of infection
Before we learn about the methods of treating neurogenic eczema, it is very important to know the factors that increase the probability of infection in order to avoid infection, as there are many factors that increase the probability of developing neurogenic eczema, whether they are psychological, physical, or environmental factors, and the following are the most prominent of these factors:
- Psychological stress and constant tension. Stress is considered one of the most important triggers for the onset or worsening of symptoms. Stress directly affects the response of the nervous system and skin.
- Anxiety and sleep disorders, as itching increases at night, and insomnia leads to increased scratching unconsciously.
- Repeated scratching or rubbing of the skin, whether as a habitual behavior or in response to anxiety, leads to skin irritation and the beginning of the inflammatory cycle.
- The presence of other chronic skin diseases such as atopic eczema or psoriasis that make the skin more susceptible to damage.
- Dry or cold weather helps dry out the skin and increases the urge to scratch.
- Wearing uncomfortable clothes or made of synthetic fabrics that cause friction on the skin and increase irritation.
- Exposure to irritating or allergenic substances, such as some types of soap, perfumes, or detergents.
How can neurogenic eczema be diagnosed?
If you suffer from symptoms of neurogenic eczema, visit Al Mousa Specialist Hospital to have the doctor diagnose neurological eczema through a clinical examination and direct observation of the symptoms by a dermatologist. The diagnosis depends on a set of steps, which are as follows:
- The doctor asks about the onset of symptoms, their severity, the pattern of itching, the presence of any accompanying psychological factors such as stress or anxiety, in addition to medical or skin history.
- Examine the skin carefully, focusing on the shape of the spots, their location, the thickness of the skin, any change in color, or signs of frequent scratching.
- Exclude other skin diseases such as psoriasis, atopic eczema, fungi or allergies, as symptoms are sometimes similar and need to be carefully differentiated.
- Ask the patient about nervous habits, such as rubbing the skin or scratching during stress, which are common behaviors among people with neurogenic eczema.
- In some cases, additional tests such as skin analysis or a small biopsy are performed if symptoms are not clear or another disease is suspected.
- Evaluating the patient's psychological state: Because diagnosis includes linking physical symptoms and psychological factors, the patient may be referred to a psychologist when needed.
Methods of treating neurogenic eczema
Of course, one unavoidable question comes to your mind now, which is: What are the approved treatment methods to get rid of the problem of neurological eczema?
- Topical treatment, which includes topical cortisone, which is used to quickly reduce inflammation and itching, moisturizing and soothing ointments to maintain skin moisture and prevent dryness, and anti-itch medications such as creams containing menthol or camphor.
- Treatment with oral medications includes antihistamines to reduce itching, especially at night and improve sleep, antidepressants or anti-anxiety medications in cases associated with psychological disorders, and oral cortisone or injections in very severe cases and under medical supervision.
- Behavioral and psychological therapy includes psychotherapy sessions or cognitive behavioral support (CBT) to help the patient manage stress and anxiety, and learn relaxation techniques such as meditation or deep breathing exercises.
- Change daily habits, such as avoiding scratching the skin as much as possible, wearing comfortable cotton clothes, and using gentle, fragrance-free soap.
- Phototherapy is sometimes used in chronic cases and depends on exposing the skin to ultraviolet rays under medical supervision.
- Continuous follow-up with a dermatologist to evaluate the effectiveness of treatment and modify the plan according to the improvement of symptoms.
Within the framework of Al Mousa Specialist Hospital’s interest in providing comprehensive medical care that combines physical and mental health, it provides Rafah Center for Mental Health Advanced services help patients alleviate the symptoms of neurological eczema and improve their quality of life. The center includes a multidisciplinary team of dermatologists and psychiatrists, and relies on cognitive behavioral therapy and relaxation techniques to reduce psychological stress, which is one of the main factors in worsening the skin condition. The center also provides a carefully designed therapeutic environment that includes outpatient clinics and inpatient units equipped with 24 individual rooms to ensure the comfort of privacy and inner peace during treatment.
Frequently asked questions
Does eczema have anything to do with the psychological state?
Yes, neurological eczema is closely related to the psychological state, as stress and anxiety are among the most prominent factors stimulating the appearance or increase of symptoms. This condition is classified as a skin disorder of neurological or psychological origin, so controlling psychological stress is an essential part of treatment.
Is eczema contagious?
No, neurogenic eczema is not contagious at all. It is a condition resulting from an interaction between the skin and the nervous system, and it is not transmitted from one person to another, whether through touching, sharing tools, or any other means.
Does neurogenic eczema go away?
Symptoms may disappear or improve for long periods when appropriate treatment is followed and triggering factors are avoided, but it is considered a chronic condition that tends to recur, especially during periods of stress. Therefore, it is important to adhere to daily skin care and control psychological stress to reduce relapses.
Our team at Al Mousa Specialist Hospital includes an elite group of dermatologists and specialists in behavioral psychotherapy to provide comprehensive and integrated care for your condition. Book your appointment today and begin your recovery journey.
المصادر:
Neurodermatitis – nationaleczema
Neurodermatitis – clevelandclinic
